The US Supreme Court gave Bayer AG a mixed reception on its bid to stop tens of thousands of lawsuits claiming its Roundup herbicide should have been labeled as a…
An Overview of Some COVID Related Impacts on Rural America from USDA’s Economic Research Service
Last week, the USDA’s Economic Research Service (ERS) released its annual report exploring characteristics and economic indicators associated with Rural America: “Rural America at a Glance: 2020 Edition.” This year’s edition of the report focused on COVID-19 related conditions and the pandemic’s impact on the rural economy. Today’s update includes highlights from the report, which was written by John Cromartie, Elizabeth Dobis, Thomas Krumel, David McGranahan, and John Pender.
The report noted that, “With 14 percent of the adult population, rural areas had about 14 percent of total confirmed COVID-19 cases and 11 percent of all deaths as of November 1, 2020. However, the rural share of cases and deaths increased markedly over time as the virus spread.
In the 3 weeks leading up to November 1 (i.e., the last 3 weeks of October), rural residents accounted for 21 percent of new cases. COVID-19 deaths became even more concentrated in rural areas, with rural residents accounting for 27 percent of the nation’s deaths from COVID-19 during the last 3 weeks of October.
“Several factors likely contributed to the higher recent rural share of COVID-19 deaths than cases, including a population that is older and living farther away from hospitals, more likely to have underlying health issues, and less likely to have health insurance.”
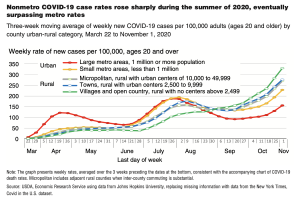
The authors explained that, “Rural rates of COVID-19 mortality were never previously higher than they were in late October, and the rise in cases during this period suggests that rural mortality is likely to continue increasing. In contrast, rates in large metro areas were the lowest since the beginning of the pandemic, although their recent rise in case rates suggests that this situation may change.”
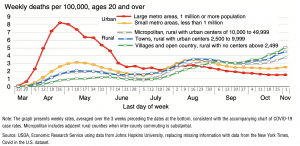
“Nonmetro population characteristics and hospital distance indicate ways the rural population is more vulnerable to severe illness or death from COVID-19 infection than the metro population,” the report said (table below).
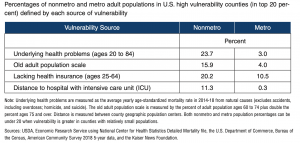
In a closer look at proximity to health care facilities, the authors pointed out that, “Some COVID-19 patients can quickly develop serious symptoms, and rural residents who are remote from intensive care hospitals may have difficulty receiving care in a timely manner. The map [below] shows nonmetro counties in the 20 percent of counties with the longest average distance to an intensive care hospital. On average, the residents of these counties are more than 32 miles from such a hospital.”

BREAKING: Covid has now killed a larger portion of people in #rural areas than in big cities -- or any other areas. https://t.co/trZ2cOGayp @nquerolo via @business #COVID19 pic.twitter.com/uO8dI2JlfA
— Mike Dorning (@MikeDorning) December 21, 2020
With respect to the economic impacts of the pandemic, the report stated that, “Nonmetro unemployment rates tracked slightly higher than in metro areas during the Great Recession of 2008-09 and throughout the 2010s but have been lower during the pandemic.”
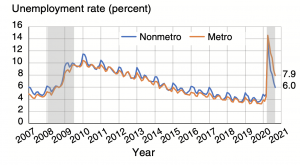
More narrowly, the ERS update also focused on COVID impacts in meatpacking-dependent counties.
The ERS authors indicated that, “The 2-week moving average number of new daily cases rose in meatpacking-dependent counties through the remainder of April, reaching a peak of nearly 50 cases per 100,000 population by the end of the month, more than 10 times the prevalence seen in other rural counties.
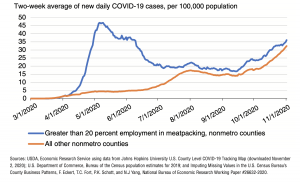
“Even though cases in meat- packing-dependent counties started to decline in May, they remained significantly higher compared to other rural counties, falling to just under 7 times the number of average daily cases per 100,000 population by the end of May. Partial plant closures and increased social distancing protocols were implemented at meatpacking plants across the country starting in late May. These measures appear to have slowed infection rates, as June saw a sharp reduction in cases in meatpacking-dependent counties.”





